Who was Claire Wineland?
Claire Wineland (photographed below) was an American activist and author who set up a non-profit organisation, “Claire’s Place Foundation”. Having cystic fibrosis herself, she wanted to help support others with terminal or chronic illnesses as well as their families. Claire had a successful double-lung transplant on the 26th of August this year. Sadly, this led to a stroke caused by a blood clot which cut off blood supply to the right side of her brain, which killed Claire on the 2nd of September 2018. Although her passing was not a direct result cystic fibrosis, this is an extremely difficult disease to live with and is often misunderstood.

Figure 1 – Claire Wineland – (Image taken from http://www.wpsdlocal6.com).
What Exactly is Cystic Fibrosis?
Cystic fibrosis (CF) is an autosomal recessive genetic disorder, meaning both parents must have the defected gene in order for their offspring to have it. It is often associated with the lungs, but actually, the name itself refers to its effects on the pancreas. Cystic refers to the cysts, or fluid-filled sacs, that form on the pancreas, and fibrosis refers to the excess connective tissue. It is caused by the mutation of the gene that encodes a chloride-conducting transmembrane channel, known as the cystic fibrosis transmembrane conductance regulator (CFTR). This gene codes for the CFTR protein, which functions as a pump for chloride ions into various secretions to thin them out.
The Mutation for CF
Although there are over 2000 variations of mutations for CFTR, the most common mutation is the ∆F508 mutation. This means a deletion of phenylalanine at the 508th amino acid. This mutated protein then gets misfolded so that it cannot migrate from the endoplasmic reticulum to the cell membrane. Hence, there is a lack of the CFTR protein on the endothelial surface, meaning chloride ions cannot be pumped out and water does not get drawn in, resulting in overly thick mucus secretions.
The Impact of CF on the Pancreas
With regards to the pancreas, pancreatic insufficiency arises in CF as a result of thick secretions blocking the pancreatic ducts. This prevents digestive enzymes from reaching the small intestine, meaning fat and protein cannot be absorbed as they cannot be broken down, leading to weight gain. This can be controlled, to an extent, through a careful diet. Damage of the pancreas itself is engendered by the blockage, as enzymes start to degrade the cells that line the pancreatic duct. This causes local inflammation, resulting in acute pancreatitis. In cases where cysts and fibrosis develop on the pancreas, this is chronic pancreatitis.
The Impact of CF on the Lungs
Lung-related issues tend to occur later on in childhood. Since the mucus becomes too thick, as shown in Figure 2 below, mucocilliary action in the airways is deprived, meaning harmful bacteria are able to colonise the lungs as they are not being expelled. This leads to coughing, fever and decreased lung function. Antibiotics can be administered to control this, however, certain bacteria become resistant and the biofilm that surrounds these bacteria protect it from being killed by antibiotics. This can then lead to bronchiectasis, which is where the airway wall is damaged and there is permanent dilation of the bronchi. Over time, this can cause respiratory failure, which is the leading cause of death for people with CF.
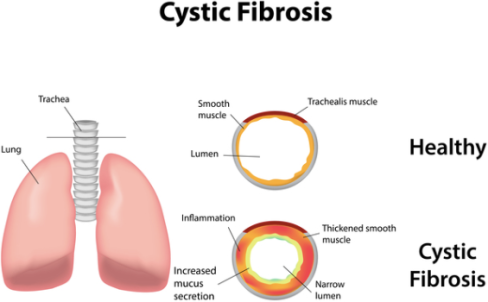
Figure 2 – The effects of cystic fibrosis on the trachea. (Image taken from www. ghr.nlm.nih.gov).
Current Treatments for CF
In terms of treatments for CF, there is a large focus on nutrition and administering supplements to aid healthy weight gain, such as replacement pancreatic enzymes. Since CF is an obstructive disease, pulmonary function tests are regularly taken to monitor the status of the disease. Pulmonary treatment involves inhalers and chest physiotherapy. As far as medications go, n-acetylcysteine can be given to CF patients as it cleaves disulphide bonds in mucus glycoproteins, as well as dornase alfa, a nuclease which cuts up nucleic acid in mucus. In severe cases, a lung transplant is carried out.
The Future for CF
Currently, there are a number of ongoing research projects and clinical trials that aim to alleviate the symptoms of CF and prolong life of those suffering from it. One particularly interesting approach is the targeting of the CFTR mutation itself. Present-day research is focussed on three groups of drugs: potentiators, correctors or read-through agents. Potentiators enhance CFTR channel activity if it is correctly located. The idea behind this is that defects such as protein misfolding in F508del are corrected, allowing trafficking to the cell surface. Read-through agents allow the ribosome to ‘ignore’ a premature termination codon and produce a full-length protein. Several of these types of drugs have progressed through clinical trials and research in CF continues to be widespread.
Claire’s Legacy
For Claire, she inspired many who suffered from any form of terminal illness. Not only did she publish her book, Every Breath I Take, but she also talked about facing the challenges of death through her YouTube channel and even gave a TEDx talk, which touched many people. Her focus was more on getting the most out of life rather than focussing on her illness and how to avoid death. Even though her passing was a tragedy, Claire’s legacy has left a huge mark on the world in terms of raising awareness of cystic fibrosis, but also living life to the fullest.
Visit http://clairesplacefoundation.org/ to donate to families struggling to support loved ones with a terminal illness.
Written by Laura
References
Edmondson, C. and Davies, J. (2016). Current and future treatment options for cystic fibrosis lung disease: latest evidence and clinical implications. Therapeutic Advances in Chronic Disease, 7(3), pp.170-183.
Elborn, J. (2016). Cystic fibrosis. The Lancet, 388(10059), pp.2519-2531.
Reference, G. (2018). Genetics Home Reference, Your Guide to Understanding Genetic Conditions. [online] Genetics Home Reference. Available at: https://ghr.nlm.nih.gov [Accessed 9 Oct. 2018].
WPSD Local 6. (2018). WPSD Local 6 – Your News, Weather, & Sports Authority. [online] Available at: https://www.wpsdlocal6.com/ [Accessed 9 Oct. 2018].
